BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
URL: http://jsurgery.bums.ac.ir/article-1-129-en.html
Endovascular treatment of Arteriovenous Graft Pseudoaneurysm: a case report
Hossein Najd Sepas1, Pooya Derakhshan2, Adnan Tizmaghz3*
1Assistant Professor of Vascular Surgery, Department of Surgery, Iran University of Medical Sciences, Tehran, Iran
2Assistant Professor of Anesthesiology, Department of Anesthesiology, Iran University of Medical Sciences, Tehran, Iran
3General Surgeon, Department of Surgery, Iran University of Medical Sciences, Tehran, Iran
Received: October 31, 2017 Revised: November 05, 2018 Accepted: August 20, 2018
|
Abstract Arteriovenous graft fistula (AVG) is used in chronic hemodialysis patients. Depending on graft materials, AVG is associated with common complications that may need several interventions. Pseudoaneurysm is one of the rare complications with various reasons. Patients with this complication require access revision and even surgical repair. However, a new method using covered-stent graft may be applied in several cases. In this study, we presented a young male hemodialysis patient with AVG referred with a pseudoaneurysm and treated with covered-stent graft. After a year, he was referred with pseudoaneurysms on two separate occasion of AVG. He was again treated with covered-stent graft. Key Words: Arteriovenous graft, Pseudoaneurysm, Stenting |
Introduction
Pseudoaneurysm endangers access and requires interventions including surgical revision or using covered-stents, as a new method. Treatment options for pseudoaneurysm include open surgery and endovascular surgical techniques (3). In the open surgical technique, the false aneurysm should be removed and a new graft is needed. The endovascular treatment is the insertion of a covered-stent graft into the arteriovenous graft fistula (AVG).
Small published series have described the arteriovenous fistula (AVF) or AVG failure or non-maturing. Most of the studies focused on the traditional forearm radiocephalic AV fistula (4). This study was conducted to report salvage procedures in the management of nonfunctional AV thigh graft and the prolongation of its lifespan.
Cases
A 10-year-old male was referred to the emergency unit with a grossly swollen right thigh. He had AVG for 3 years without any problem during hemodialysis. However, he recently presented with a giant pseudoaneurysm in the right thigh, as well as the compromise of overlying skin. He had hypertension in his medical history and pulmonary hypertension because of poor cardiac conditions. He underwent endovascular treatment using
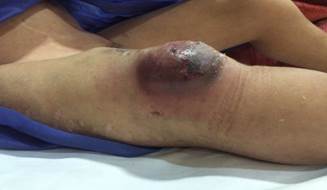
Figure 1: A large pseudoaneurysm with overlying skin ischemia of the right thigh
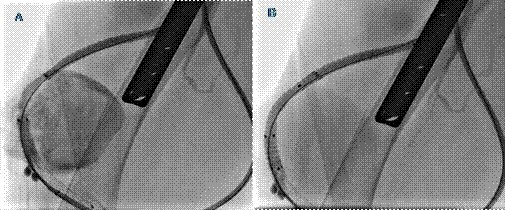
Figure 2: (A) Venogram demonstrating an arteriovenous graft pseudoaneurysm. (B) venogram showing a fully excluded arteriovenous graft pseudoaneurysm by the covered-stent
Hemodialysis was performed successfully twice and he was later discharged in good condition. After a year, the patient presented with recurrent symptoms and pseudoaneurysm in two sites of AVG fistula. He was again treated with covered-stent graft and the graft became functional again (Figure 2).
Discussion
A well-functioning vascular access (VA) is essential for an efficient hemodialysis. There are three major types of VA, namely, native AVF, AVG, and central venous catheter. The AVF remains the first choice long-term VA for hemodialysis (5). Moreover, AVG creation is the second step of treatment, following the AVF made with native vessels (6). Further evaluations are necessary in case of VA dysfunctions in hemodialysis patients.
Color Doppler ultrasound is the first tool in the assessment of functional and structural problems of VA, cause of failure, correctability, or salvage, and determination of alternative sites (7). Patients with VA dysfunctions present with sub-optimal dialysis or extremity swelling secondary to catheter-related deep venous thrombosis. A Doppler ultrasonography can easily identify the latter veins. In this case, endovascular treatment is considered to reestablish deep venous outflow following catheter removal.
Subsequent imaging is directed at assessing the efficacy of treatment and identifying an alternative insertion site (4). The surgical management of VA dysfunction provides better life expectancy than endovascular approach and should be used when indicated (8). Small published series have focused on reintervention of failing or non-maturing AV autogenous accesses. Hingorani et al. reported their experience with salvage procedures for the correction of nonfunctional upper arm AV fistulas. In 46 patients (49 fistulas), 75 procedures were performed, out of whom 17 patients underwent 26 balloon angioplasties, and 20 patients had vein patch angioplasty. The group performed 12 fistula revisions to a more proximal level and four vein interposition grafts. There was no significant difference between primary patency rates of open surgical repair and endovascular correction.
They concluded that salvage procedures may allow maturation and better longevity of AV fistulas for hemodialysis (9). Berman and Gentile reported a 90% functional access achievement in patients during secondary interventions on the maturation and maintenance of autogenous AV fistulas (10). If upper extremity options are dissatisfying and the superior central venous system is obstructed, lower extremity access options can be used (11).
The transposition of the saphenous vein in a loop configuration to the superficial or common femoral artery has been conducted. As another option, a prosthetic bypass graft can be placed in a loop configuration from the common femoral vein to the superficial or common femoral artery. A prosthetic bypass graft can be created from one femoral artery to a contralateral femoral vein and tunneled subcutaneously across the lower anterior abdominal wall (12).
Conclusions
Endovascular repair of AVG pseudoaneurysm is a safe, simple, and effective procedure to prevent further growth and decrease the probability of rupture, leading to increased AVG functional lifespan.
Acknowledgments
We thank all of the participants in this study for their cooperation.
Consent
All authors declare that written informed consent was obtained from the patient for publication of this report.
Conflict of Interest
There is no conflict of interest to be declared.
References
1. Marzelle J, Gashi V, Nguyen HD, Mouton A, Becquemin JP, Bourquelot P. Aneurysmal degeneration of the donor artery after vascular access. J Vasc Surg. 2012; 55(4):1052-7. DOI: 10.1016/j.jvs.2011.10.112
2. Barshes NR, Annambhotla S, Bechara C, Kougias P, Huynh TT, Dardik A, et al. Endovascular repair of hemodialysis graft-related pseudoaneurysm: an alternative treatment strategy in salvaging failing dialysis access. Vasc Endovascular Surg. 2008; 42(3):228-34. DOI: 10.1177/1538574408314443
3. Najibi S, Bush RL, Terramani TT, Chaikof EL, Gunnoud AB, Lumsden AB, et al. Covered stent exclusion of dialysis access pseudoaneurysms. J Surg Res. 2002; 106(1):15-9.
4. Townsend CM, Beauchamp RD, Evers BM, Mattox KL. Sabiston textbook of surgery: New York: Elsevier Health Sciences; 2012.
5. Santoro D, Benedetto F, Mondello P, Pipitò N, Barillà D, Spinelli F, et al. Vascular access for hemodialysis: current perspectives. Int J Nephrol Renovasc Dis. 2014; 7:281-94. DOI: 10.2147/IJNRD.S46643
6. Stehman-Breen CO, Sherrard DJ, Gillen D, Caps M. Determinants of type and timing of initial permanent hemodialysis vascular access. Kidney Int. 2000; 57(2):639-45. DOI: 10.1046/j.1523-1755.2000.00885.x
7. Riella MC, Roy-Chaudhury P. Vascular access in haemodialysis: strengthening the Achilles' heel. Nat Rev Nephrol. 2013; 9(6):348-57. DOI: 10.1038/
nrneph.2013.76
8. Vachharajani TJ. Diagnosis of arteriovenous fistula dysfunction. Semin Dial. 2012; 25(4):445-50. DOI: 10.1111/j.1525-139X.2012.01094.x
9. Hingorani A, Ascher E, Kallakuri S, Greenberg S, Khanimov Y. Impact of reintervention for failing upper-extremity arteriovenous autogenous access for hemodialysis. J Vasc Surg. 2001; 34(6):1004-9. DOI: 10.1067/mva.2001.119750
10. Berman SS, Gentile AT. Impact of secondary procedures in autogenous arteriovenous fistula maturation and maintenance. J Vasc Surg. 2001; 34(5):866-71. DOI: 10.1067/mva.2001.118086
11. Silva MB Jr, Hobson RW 2nd, Pappas PJ, Jamil Z, Araki CT, Goldberg MC, et al. A strategy for increasing use of autogenous hemodialysis access procedures: impact of preoperative noninvasive evaluation. J Vasc Surg. 1998; 27(2):302-8.
12. Pierre-Paul D, Williams S, Lee T, Gahtan V. Saphenous vein loop to femoral artery arteriovenous fistula: a practical alternative. Ann Vasc Surg. 2004; 18(2):
223-7. DOI: 10.1007/s10016-004-0016-7
Received: 2017/10/31 | Accepted: 2018/08/20 | Published: 2018/11/14 | ePublished: 2018/11/14
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |







