BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
URL: http://jsurgery.bums.ac.ir/article-1-158-en.html

 , Ahmad Amouzeshi
, Ahmad Amouzeshi 

 , Mostafa Behmanesh
, Mostafa Behmanesh 
 , Ali Mohammad Pourbagher-Shahri
, Ali Mohammad Pourbagher-Shahri 

 , Soroush Hozeifi
, Soroush Hozeifi 

 , Ali Rajabpour-Sanati *
, Ali Rajabpour-Sanati * 


Comparison of the effect of diclofenac suppository with intravenous meperidine in relieving pain after laparoscopic cholecystectomy in opioid-dependent and independent patients
Mohammad Yarani1, Ahmad Amouzeshi2 , Mostafa Behmanesh3, Ali Mohammad Pourbagher-Shahri3
, Mostafa Behmanesh3, Ali Mohammad Pourbagher-Shahri3 , Soroush Hozeifi3
, Soroush Hozeifi3 , Ali Rajabpour-Sanati3*
, Ali Rajabpour-Sanati3*
1Assistant Professor, Department of Surgery, Birjand University of Medical Sciences, Birjand, Iran
2Associate Professor, Department of Cardiac Surgery, Birjand University of Medical Sciences, Birjand, Iran
3Faculty of Medicine, Birjand University of Medical Scienes, Birjand, Iran
Received: October 08, 2018 Revised: September 17, 2019 Accepted: September 17, 2019
|
Abstract Introduction: Cholecystitis is one of the most common diagnoses among patients referred to surgical emergencies with acute or recurrent abdominal pain. The mainstay of treatment for this disease is cholecystectomy, and the gold standard procedure is laparoscopic cholecystectomy. Pain which is the most common complication after laparoscopic cholecystectomy gives priority to the administration of the best pain relief medicine. This study aimed to compare the efficacy of diclofenac suppository with intravenous Meperidine for pain relief in opioid-dependent and independent patients undergoing laparoscopic cholecystectomy. Methods: A total of 120 opioid-dependent and independent patients (60 each) participated in this single-blinded study. Each group was randomly divided into two equal subgroups and 100 mg diclofenac suppository and 25 mg Meperidine via intravenous injection were administered to the participants in each group. Pain intensity was measured by the Verbal Rating Scale (VRS) pain scale 24 hours after recovery. The data were analyzed in SPSS software (version16.0). P-value less than 0.05 was considered statistically significant. Results: Based on the results of the study, Meperidine for pain relief after laparoscopic cholecystectomy was reported to be more effective in opioid-dependent patients and diclofenac in opioid-independent patients. Moreover, the use of diclofenac in 90% of opioid-independent patients resulted in favorable responses and ease of pain (Fisher=61.01; P=0.001), and the rate of opioid-dependent patients treated with Meperidine with excellent responses were measured at 83.3% (Fisher=56.98, P=0.001). Conclusions: Meperidine can be the mainstay of treatment for pain relief after laparoscopic cholecystectomy used in opioid-dependent patients; however, the selected drug for pain relief after laparoscopic cholecystectomy in opioid-independent patients is diclofenac. Key words: Cholecystectomy, Diclofenac, Laparoscopy, Meperidine, Pain management |
Introduction
Gallstone disease is a major health concern the world over. Gallstones are hardened deposits of the digestive fluid bile which can form within the gallbladder(1, 2). In developed countries, the prevalence of gallstones among the adult population ranges from 10-15% and independent factors contributing to their development include family history, genetic predisposition, ethnic background, female gender, and age(3-5). Most gallstones remain asymptomatic; however, up to 25% of them become symptomatic in the form of cholecystitis, cholangitis, or biliary pancreatitis (6). When a patient develops symptoms or complications related to gallstones, surgical treatment remains the gold standard due to the high rate of medical re-admission (7) due to the same symptoms or pancreatitis or cholecystitis within a discrete-time frame. Furthermore, biliary colic is one of the most common precursors of life-threatening gallstone-related complications(8-10). In recent years, non-aggressive efforts have been made to treat gallstones as lithotripsy by electric waves and drug therapy for the elimination
of biliary salts (11). Open or laparoscopic cholecystectomy produces desirable long-term outcomes in patients with symptomatic stones; therefore, about 90% of patients with specific symptoms of gallstones after cholecystectomy are asymptomatic. Laparoscopic cholecystectomy is a common surgical procedure nowadays, in the United States, for instance, 90 percent of surgeries are laparoscopic cholecystectomy (12). According to different health care systems, the recent data has revealed that consensus on a strategy favoring early laparoscopic cholecystectomy is very cost-effective(13-15). Laparoscopic cholecystectomy took the place of open cholecystectomy as the gold standard treatment for gallstones(16). Although the laparoscopic procedure requires more operating time than the open procedure, it has many advantages over open cholecystectomy, such as no need of cutting the rectus abdominal muscle, less pain after surgery, shorter period of hospitalization, less incisional hernia, more beauty, and a faster return to work and social functioning (17). Moreover, severe complications of laparoscopic cholecystectomy are rare, and mortality rate of laparoscopic cholecystectomy is less than open cholecystectomy (about 0.1 percent). In addition, wound infection and heart-lung disease after laparoscopic cholecystectomy are much less, as compared to open procedures; however, the damage to extrahepatic biliary
tract is more common (18, 19). Laparoscopic cholecystectomy is now considered the gold standard therapy for symptomatic cholelithiasis and chronic cholecystitis (20). All of the mentioned merits have made laparoscopic cholecystectomy a more efficient method with higher satisfaction among patients; however, it has some side effects. Although due to smaller incision, intercostal nerves and muscles of the abdominal wall are less painful than open surgery, there are still different causes of pain after surgery in these patients (21, 22). Furthermore, one of the main concerns of surgeons is finding a way to better control post-surgical pain since the duration of hospital stay plays an essential role in pain, patient satisfaction, convalescence, and return to usual activities(23-26). Postoperative pain control methods include the regular use of selective and non-selective NSAID (a nonsteroidal anti-inflammatory drug), topical anesthetics, and intravenous opioids, such as morphine, meperidine, steroids, and clonidine (22, 24, 27-32). However, opioids which are used to control post-surgical pain as a routine procedure, especially in the early hours after surgery was associated with some restrictions (33). Nonselective NSAID is another batch of drugs widely used to control postoperative pain in the process (34-36). However, these drugs carry their own pitfalls and serious complications especially if used for the management of acute pain. This can be attributed to their effects on inhibition of Cyclooxygenase-I, and Cyclooxygenase-II in combination with their anti-inflammatory and analgesic activity. These complications include increased risk of bleeding in the upper gastrointestinal tract, acute renal failure, impaired platelet function followed by severe bleeding during or after surgery. Following these complications, COX-II-selective NSAIDs are more prefered than COX-II-non-selective NSAIDs in patients who are susceptible to upper gastrointestinal bleeding(37). Many studies have been conducted on finding the best way to control pain after laparoscopic cholecystectomy. Joshi et al. (38) in a study conducted on 263 patients determined the effect of Parecoxib intravenous dose before surgery and continued oral therapy with Valdecoxib for the treatment of pain associated with elective laparoscopic cholecystectomy and their impact on the reduction of the need for opioids. The result of the mentioned study signified a 21% reduction of fentanyl administration in the patients who received Parecoxib, as compared to the placebo group. On the other hand, patients who received Valdecoxib after hospital discharge needed fewer analgesics supplements. In addition, the incidence of adverse effects in Parecoxib and Valdecoxib group was less, as compared to the placebo group (38). In another study, Cheng et al. (39) evaluated the effectiveness of Celecoxib in the reduction of opioids consumption in patients undergoing laparoscopic cholecystectomy. The results of this study revealed that pain scores and morphine consumption in the two treatment groups were not statistically significant. Celecoxib can reduce opioid use to reduce pain in patients who had a laparoscopic cholecystectomy, and the combination of several techniques to relieve multi-factorial
pain following laparoscopic cholecystectomy is
more efficient (39). Ariana and Rafei compared
the postoperative analgesia in laparoscopic cholecystectomy using two methods, including bupivacaine in peritoneal and intravenous Meperidine. The results of the mentioned study suggested that oral analgesic requirements in the bupivacaine group were significantly lower than that of intravenous Meperidine. Moreover, nausea and vomiting in the first few hours in bupivacaine group were lower than that of intravenous Meperidine, and the patient's breathing in the peritoneal bupivacaine group was higher than that of intravenous Meperidine (40). Soroush et al. in a study evaluated the effectiveness of Celecoxib in the reduction of pain in patients after laparoscopic cholecystectomy. The results showed that celecoxib administration before and after surgery had a significant effect on the reduction of analgesic consumption. The mean pain score showed a significant difference between the treatment group and the control group. In addition, a significant difference was observed between the treatment group and the control group concerning post-surgical nausea and vomiting, the length of hospital stay, and intestinal function (37). The results of the study performed by Abdollahi et al. on the effect of two analgesic medication, including diclofenac suppository, and Meperidine on pain relief after inguinal hernia surgery, no statistically significant difference was observed between the two groups in terms of pain relief in the first 24 hours after surgery. According to the results of this study, diclofenac sodium can be used as an alternative to Meperidine to relieve pain after inguinal hernia surgery (41). Despite the importance of post-surgical pain management and many studies performed in this field, selecting the right medication for the achievment of the optimal analgesia based on patient's condition, espicially in addicted patients poses clinical challenges to the physicians. The relatively high prevalence of opioid substances can lead to the development of tolerance to this group of drugs in patients (42). Moreover, different protocols are used in different medical centers for pain management after laparoscopic cholecystectomy. This study aimed to compare the efficacy of diclofenac as a NSAID with the intravenous Meperidine as opioid in pain relief in opioid-dependent (OD) and opioid-independent (OI) patients undergoing laparoscopic cholecystectomy after the surgery.
Methods
This clinical trial was approved by the ethics committee of Birjand University of Medical Sciences with “Ir.Bums.Rec.1394.244” code, and
in Iranian registry of clinical trials with “IRCT20140611018063N6” code. The current study was conducted as a single-blinded clinical trial and a patients' pain intensity was evaluated by a nurse who did not know the prescribed drug (blind) using Verbal Rating Scale (VRS) pain scale. The sample size was estimated as 60 patients for each group (120 patients total) based on the study conducted by Soroori et al. (43), and α=0.05, and β=0.2 were calculated using the following formula:
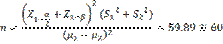
The study population included the patients diagnosed with gallstones or biliary sludge and requiring surgery who were admitted to Imam Reza hospital in Birjand from November 2015
to April 2016 and all of them underwent laparoscopic cholecystectomy. Participants who were selected by convenience sampling method were enrolled in the study after adjusting for age, gender, and other demographic variables. Thereafter, the participants were provided with the purpose of the study and the written informed consent was obtained from all of them. Exclusion criteria entailed: the presence of laparoscopic cholecystectomy, relative contraindications, such as severe obstructive pulmonary disease, congestive heart failure (EF <20%), acute cholecystitis, gangrenous and empyema gallbladder, intestinal fistula in the biliary tract, obesity, pregnancy, ventriculoperitoneal shunt and cirrhosis, previous abdominal surgery, and appearance of serious drug side effects. The subjects in each group (n=60) were randomly assigned into two equal subgroups (A and B). All patients underwent laparoscopic cholecystectomy under general anesthesia. One subset of each opioid-dependent and opioid-independent patients were given 100 mg Diclofenac suppository through the rectal and other subgroups were given 25 mg

Figure 1: Flow diagram of patients
Meperidine injection intravenously. The drug administration initiated an hour after the recovery and continued every 6 hours for 24 hours. Due to the increased half-life of Meperidine to 1.3 to 2 fold, as well as to the decreased gastrointestinal movements in post-operative patients (44), the lowest possible dose for Meperidine was selected.
Pain intensity was evaluated by a nurse who was blind to the prescribed drug 24 hours after the administration of drugs using a VRS pain scale. The data were analyzed in SPSS software (version16) regarding descriptive indexes (mean, standard deviation, frequency, and percentage). The relationship between variables was examined using Chi-square and Fisher’s exact tests at the significance level of 0.05 (Figure 1).
Results
A total of 120 patients participated in the current study after the implementation of the exclusion criteria and all of them completed the study. Based on the obtained results, 43.3 %( n=52) of the participants did not experience any pain after the drug administration (excellent response to the drug), regardless of gender, type of drug and opioid dependency or independency (Table 1). After separation of patients based on dependency on opioid, 27 patients (45%) in the opioid-independent group did not go through any pain after drug treatment; however, this value was measured at 41.7% in opioid-dependent patients (Table 2). Moreover, the separation of patients by
Table 1: Overall distribution of patients undergoing laparoscopic cholecystectomy in terms of pain severity
|
Severity of pain (response to treatment) |
Frequency |
Percent |
|
Severe pain (without response) |
29 |
24.2 |
|
Moderate Pain (Moderate response) |
9 |
7.5 |
|
Mild pain (good response) |
30 |
25.0 |
|
Painless (excellent response) |
52 |
43.3 |
|
Total |
120 |
100 |
Table 2: Distribution of patients undergoing laparoscopic cholecystectomy in terms of pain severity, based on opioid dependency
|
|
Severity of pain (response to treatment) |
Frequency |
Percent |
|
Opioid-independent patients |
Severe pain (without response) |
21 |
35.0 |
|
Moderate Pain (Moderate response) |
4 |
6.7 |
|
|
Mild pain (good response) |
8 |
13.3 |
|
|
Painless (excellent response) |
27 |
45.0 |
|
|
Total |
60 |
100 |
|
|
Opioid-dependent patients |
Severe pain (without response) |
8 |
13.3 |
|
Moderate Pain (Moderate response) |
5 |
8.3 |
|
|
Mild pain (good response) |
22 |
36.7 |
|
|
Painless (excellent response) |
25 |
41.7 |
|
|
Total |
60 |
100 |
Table 3: Distribution of patients undergoing laparoscopic cholecystectomy in terms of pain severity, based on types of prescribed drugs
|
|
Severity of pain (response to treatment) |
Frequency |
Percent |
|
Diclofenac |
Severe pain (without response) |
11 |
18.3 |
|
Moderate Pain (Moderate response) |
5 |
8.3 |
|
|
Mild pain (good response) |
17 |
28.3 |
|
|
Painless (excellent response) |
27 |
45.0 |
|
|
Total |
60 |
100 |
|
|
Meperidine |
Severe pain (without response) |
18 |
30.0 |
|
Moderate Pain (Moderate response) |
4 |
6.7 |
|
|
Mild pain (good response) |
13 |
21.7 |
|
|
Painless (excellent response) |
25 |
41.7 |
|
|
Total |
60 |
100 |
prescribed drug indicated that 45% (n=27) of patients in diclofenac group and 41.7% (n=25) of patients in Meperidine group felt no pain after
the treatment (Table 3). However, after the separation of patients by opioid independency, as well as types of drugs, it was signified that 90%(n=27) of opioid-independent patients who take diclofenac felt no pain after drug administration, and 8 patients (26.7%) went through mild pain, and none of the patients were painless.
On the other hand, 56.7% (n=17) of diclofenac-user patients in opioid-dependent group experienced mild pain and no one was painless. However, 83.3% (n=25) of opioid-dependent patients who consumed Meperidine were painless after taking the drug. Comparison of pain severity after laparoscopic cholecystectomy in opioid-dependent and independent patients between the recipient of Meperidine and diclofenac revealed a significant relationship in 24 hours after surgery (P <0.05) in general Meperidine in opioid-dependent patients and diclofenac in opioid independent patients regarding the relief of pain after laparoscopic cholecystectomy (Table 4 and 5).
Table 4: Comparison of pain intensity in laparoscopic cholecystectomy in opioid-dependent and independent patients receiving Meperidine
|
|
Severity of pain (response to treatment) |
Total |
||||
|
Severe pain (without response) |
Moderate Pain (Moderate response) |
Mild pain (good response) |
Painless (excellent response) |
|||
|
opioid independent patients |
Frequency |
18 |
4 |
8 |
0 |
30 |
|
Percent |
60 |
13.3 |
26.7 |
0.0 |
100 |
|
|
opioid dependent patients |
Frequency |
0 |
0 |
5 |
25 |
30 |
|
Percent |
0.0 |
0.0 |
16.7 |
83.3 |
100 |
|
|
Total |
Frequency |
18 |
4 |
13 |
25 |
60 |
|
Percent |
30.0 |
6.7 |
21.7 |
41.7 |
100 |
|
|
“Fisher’s exact test results” Fisher=56.98 P=0.001 |
||||||
Table 5: Comparison of pain intensity in laparoscopic cholecystectomy in opioid-dependent and independent patients receiving diclofenac
|
|
Severity of pain (response to treatment) |
Total |
||||
|
Severe pain (without response) |
Moderate Pain (Moderate response) |
Mild pain (good response) |
Painless (excellent response) |
|||
|
opioid independent patients |
Frequency |
3 |
0 |
0 |
27 |
30 |
|
Percent |
10.0 |
0.0 |
0.0 |
90.0 |
100 |
|
|
opioid dependent patients |
Frequency |
8 |
5 |
17 |
0 |
30 |
|
Percent |
26.7 |
16.7 |
56.6 |
0.0 |
100 |
|
|
Total |
Frequency |
11 |
5 |
17 |
27 |
60 |
|
Percent |
18.3 |
8.3 |
28.3 |
45.0 |
100 |
|
|
“Fisher’s exact test results” Fisher=61.01 P=0.001 |
||||||
Discussion
Cholecystitis is the inflammation of the gallbladder which mostly occurs due to the obstruction of the cystic duct by gallstones arising from the gallbladder (5). Laparoscopic cholecystectomy is considered the gold standard for the surgical treatment of cholecystitis (16). Although laparoscopic cholecystectomy is associated with less postoperative pain, as compared to open cholecystectomy, it carries its own complications and is not without any pain. Many different analgesic techniques for post-laparoscopy pain relief have been evaluated (22, 23). Early pain is the most common complaint after laparoscopic cholecystectomy (22, 45). The present study was conducted on 120 patients (20% male and 80% female). This ratio is justified due to a higher incidence of cholecystitis in women (46); however, the subjects' gender little mattered for inclusion in the current study. Nearly half of the patients (43.2%) who underwent laparoscopic cholecystectomy had a good response to prescribed medicines, regardless of gender, type of drug dependence or independence. However, about a quarter of the patients (24.2%) did not respond to these drugs. In other studies, the difference in responses between opioid and non-opioid based drugs has been examined (47-49). However, in the current study, we compared their responses between OD and OI patients. Similar results were obtained in the study performed by Taghinejad et al. on the effect of Meperidine hydrochloride and diclofenac sodium on post-cesarean pain, diclofenac was found to reduce post-cesarean pain more effectively, as compared to the use of Meperidine hydrochloride (50). Abdollahi et al. conducted a study on the effect of two analgesic medication diclofenac suppositories with injection Meperidine in pain relief after inguinal hernia surgery. The results of the mentioned study indicated no statistically significant difference in the first 24 hours after surgery (51). Ariana and Rafei compared
the postoperative analgesia in laparoscopic cholecystectomy with two bupivacaine methods in peritoneal with intravenous Meperidine. The findings of this study suggested that oral analgesic requirements after intraperitoneal surgery in bupivacaine group were significantly lower than that of intravenous Meperidine (40). The results of the study performed by Cheng et al. (39) signified that Celecoxib administration is not effective in the reduction of opioids consumption to ease the pain of patients who had laparoscopic cholecystectomy. On the other hand, a combination of several techniques is more worthwhile in the alleviation
of multi-factorial pain following laparoscopic cholecystectomy. In our study, less than half of OD patients with either Meperidine or diclofenac treatment had an excellent response, while more than one-tenth of them had no response to the prescribed drugs. In the case of OI patients, the administration of both Meperidine and diclofenac had an excellent response in nearly half of the patients, while one-third of them had no response to the drug. Regardless of the type of administered drug, prescribed drugs evoked a comparable response in OD and OI patients regarding excellent pain relief. However, the rate of non-response to prescribed drugs in OI patients was reported to be about three times higher than that of OD patients. Regardless of the type of administrated drug, favorable response to treatment regarding the reduction of post-surgical pain after in OI patients was a bit higher, as compared to that of OD patients. On the other hand, the absence of any responses to treatment was about three times higher in OI patients, as compared to OD patients. In general, it was found that the administration of diclofenac in 90% of OI patients resulted in a favorable response and the disappearance of pain.
On the contrary, Meperidine administration evoked favorable responses in 83.3% of OD patients who inflicted no pain. In countries and areas with higher rates of opioid addictions, controlling the pain poses a drastic challenge to the medical team and patients. According to the results of this study, the use of Meperidine is more effective in the reduction of postoperative pain in OI patients, and diclofenac suppository is more worthwhile in OD patients.
It is worthy to note that a review study conducted by Abdolrazaghnejad et al. revealed
that among narcotics, morphine can be more appropriate, as compared to Meperidine regarding pain relief, especially in cases where emergency and long-term analgesia is needed (52).
It can be concluded that regardless of opioid dependency status in patients undergoing laparoscopic cholecystectomy, diclofenac suppository evoked more favorable responses, as compared to intravenous Meperidine regarding the reduction of pain. However, further studies on the effect of these two drugs are commended due to the absence of studies in this field, as well as the importance and limitations of this subject. It is also suggested that future studies use a quantitative scale rather than a qualitative scale to assess pain intensity and examine the pain at different hours of the day. Furthermore, proper studies should be designed and implemented to determine the safety and possible side effects of these drugs for better and more accurate decision-making in the process of treatment.
Conclusions
The results of the current study revealed that non-opioid drugs, such as diclofenac sodium can be used to achieve analgesia in patients and expect favorable results similar to those of opioids, contrary to popular belief in many medical centers and due to the numerous complications of opioids administration. However, in opioid-dependent patients, the results are less satisfactory and sometimes opioid drugs are needed to achieve optimal pain management.
Acknowledgments
Our sincere appreciation and thanks go to the personnel of Imam Reza Hospital for their invaluable support and contribution.
Funding
None declared.
Conflict of Interest
The authors declare that there is no conflict of interest to be declared.
References
1. Channa NA, Khand FD, Khand TU, Leghari MH, Memon AN. Analysis of human gallstones by Fourier Transform Infrared (FTIR). Pak J Med Sci. 2007; 23(4):546.
2. Njeze GE. Gallstones. Niger J Surg. 2013; 19(2):49-55. PMID: 24497751 DOI: 10.4103/1117-6806.119236
3. Schuld J, Glanemann M. Acute cholecystitis. Viszeralmedizin. 2015; 31(3):163-5. PMID: 26468309 DOI: 10.1159/000431275
4. Stinton LM, Myers RP, Shaffer EA. Epidemiology of gallstones. Gastroenterol Clin North Am. 2010; 39(2):157-69. PMID: 20478480 DOI: 10.1016/j.
gtc.2010.02.003.
5. Stinton LM, Shaffer EA. Epidemiology of gallbladder disease: cholelithiasis and cancer. Gut Liver. 2012; 6(2):172-87. PMID: 22570746 DOI: 10.5009/gnl.
2012.6.2.172.
6. Sakorafas GH, Milingos D, Peros G. Asymptomatic cholelithiasis: is cholecystectomy really needed? A critical reappraisal 15 years after the introduction of laparoscopic cholecystectomy. Dig Dis Sci. 2007; 52(5):1313-25. PMID: 17390223 DOI: 10.1007/
s10620-006-9107-3
7. Sobolev B, Mercer D, Brown P, FitzGerald M, Jalink D, Shaw R. Risk of emergency admission while awaiting elective cholecystectomy. CMAJ. 2003; 169(7):662-5. PMID: 14517123
8. Cheruvu C, Eyre-Brook I. Consequences of prolonged wait before gallbladder surgery. Ann R Coll Surg Engl. 2002; 84(1):20-2. PMID: 11892728
9. Ito K, Ito H, Whang EE. Timing of cholecystectomy for biliary pancreatitis: do the data support current guidelines? J Gastrointest Surg. 2008; 12(12):2164-70. PMID: 18636298 DOI: 10.1007/s11605-008-0603-y
10. Macafee D, Humes D, Bouliotis G, Beckingham I, Whynes D, Lobo D. Prospective randomized trial using cost–utility analysis of early versus delayed laparoscopic cholecystectomy for acute gallbladder disease. Br J Surg. 2009; 96(9):1031-40. PMID: 19672930 DOI: 10.1002/bjs.6685
11. Paumgartner G, Sauter GH. Extracorporeal shock wave lithotripsy of gallstones: 20th anniversary of the first treatment. Eur J Gastroenterol Hepatol. 2005; 17(5):525-7. PMID: 15827443 DOI: 10.1097/
00042737-200505000-00009
12. Csikesz NG, Singla A, Murphy MM, Tseng JF, Shah
SA. Surgeon volume metrics in laparoscopic cholecystectomy. Dig Dis Sci. 2010; 55(8):2398-405. PMID: 19911275 DOI: 10.1007/s10620-009-1035-6
13. Garner JP, Sood SK, Robinson J, Barber W, Ravi K. The cost of ignoring acute cholecystectomy. Ann R Coll Surg Engl. 2009; 91(1):39-42. PMID: 19126334 DOI: 10.1308/003588409X359079
14. Johner A, Raymakers A, Wiseman SM. Cost utility of early versus delayed laparoscopic cholecystectomy for acute cholecystitis. Surg Endosc. 2013; 27(1):256-62. PMID: 22773234 DOI: 10.1007/s00464-012-2430-1
15. Wilson E, Gurusamy K, Gluud C, Davidson B. Cost–utility and value‐of‐information analysis of early versus delayed laparoscopic cholecystectomy for acute cholecystitis. Br J Surg. 2010; 97(2):210-9. PMID: 20035545 DOI: 10.1002/bjs.6872
16. Wu SD, Han JY, Tian Y. Single-incision laparoscopic cholecystectomy versus conventional laparoscopic cholecystectomy: a retrospective comparative study. J Laparoendosc Adv Surg Tech A. 2011; 21(1):25-8. PMID: 21194305 DOI: 10.1089/lap.2010.0377
17. Chau CH, Tang CN, Siu WT, Ha JP, Li MK. Laparoscopic cholecystectomy versus open cholecystectomy in elderly patients with acute cholecystitis: retrospective study. Hong Kong Med J. 2002; 8(6):394-9. PMID: 12459594
18. Duca S, Bمlم O, Al-Hajjar N, lancu C, Puia I, Munteanu D, et al. Laparoscopic cholecystectomy: incidents and complications. A retrospective analysis of 9542 consecutive laparoscopic operations. HPB. 2003; 5(3):152-8. PMID: 18332976 DOI: 10.1080/
13651820310015293
19. Radunovic M, Lazovic R, Popovic N, Magdelinic M, Bulajic M, Radunovic L, et al. Complications of laparoscopic cholecystectomy: our experience from a retrospective analysis. Open Access Maced J Med Sci. 2016; 4(4):641-6. PMID: 28028405 DOI: 10.3889/
oamjms.2016.128
20. Coccolini F, Catena F, Pisano M, Gheza F, Fagiuoli S, Di Saverio S, et al. Open versus laparoscopic cholecystectomy in acute cholecystitis. Systematic review and meta-analysis. Int J Surg. 2015; 18:196-204. PMID: 25958296 DOI: 10.1016/j.ijsu.2015.
04.083
21. Macaron C, Qadeer MA, Vargo JJ. Recurrent abdominal pain after laparoscopic cholecystectomy. Cleve Clin J Med. 2011; 78(3):171-8. PMID: 21364161 DOI: 10.3949/ccjm.77a.09171
22. Wills V, Hunt D. Pain after laparoscopic cholecystectomy. Br J Surg. 2000; 87(3):273-84. PMID: 10718794 DOI: 10.1046/j.1365-2168.
2000.01374.x
23. Bisgaard T. Analgesic treatment after laparoscopic cholecystectomya critical assessment of the evidence. Anesthesiology. 2006; 104(4):835-46. PMID: 16571981 DOI: 10.1097/00000542-200604000-00030
24. Mitra S, Khandelwal P, Roberts K, Kumar S, Vadivelu N. Pain relief in laparoscopic cholecystectomy--a review of the current options. Pain Pract. 2012; 12(6):485-96. PMID: 22008277 DOI: 10.1111/j.
1533-2500.2011.00513.x
25. Singla S, Mittal G, Raghav, Mittal RK. Pain management after laparoscopic cholecystectomy-a randomized prospective trial of low pressure and standard pressure pneumoperitoneum. J Clin Diagn Res. 2014; 8(2):92-4. PMID: 24701492 DOI: 10.7860/JCDR/2014/7782.4017
26. Szental J, Webb A, Weeraratne C, Campbell A, Sivakumar H, Leong S. Postoperative pain after laparoscopic cholecystectomy is not reduced by intraoperative analgesia guided by analgesia nociception index (ANI®) monitoring: a randomized clinical trial. Br J Anaesth. 2014; 114(4):640-5. PMID: 25540069 DOI: 10.1093/bja/aeu411
27. Akaraviputh T, Leelouhapong C, Lohsiriwat V, Aroonpruksakul S. Efficacy of perioperative parecoxib injection on postoperative pain relief after laparoscopic cholecystectomy: a prospective, randomized study. World J Gastroenterol. 2009; 15(16):2005-8. PMID: 19399934 DOI: 10.3748/
wjg.15.2005
28. Lee IO, Kim SH, Kong MH, Lee MK, Kim NS, Choi YS, et al. Pain after laparoscopic cholecystectomy: the effect and timing of incisional and intraperitoneal bupivacaine. Can J Anesth. 2001; 48(6):545-50. PMID: 11444448 DOI: 10.1007/BF03016830
29. Agarwal A, Gautam S, Gupta D, Agarwal S, Singh P, Singh U. Evaluation of a single preoperative dose of pregabalin for attenuation of postoperative pain after laparoscopic cholecystectomy. Br J Anaesth. 2008; 101(5):700-4. PMID: 18716003 DOI: 10.1093/
bja/aen244
30. Louizos A, Hadzilia S, Leandros E, Kouroukli I, Georgiou L, Bramis J. Postoperative pain relief after laparoscopic cholecystectomy: a placebo-controlled double-blind randomized trial of preincisional infiltration and intraperitoneal instillation of levobupivacaine 0.25%. Surg Endosc. 2005; 19(11):1503-6. PMID: 16328673 DOI: 10.1007/
s00464-005-3002-4
31. Xiong Z, Tang Y. Pain control after laparoscopic cholecystectomy. London: Europe PMC; 2007.
32. Lepner U, Goroshina J, Samarutel J. Postoperative pain relief after laparoscopic cholecystectomy: a randomised prospective double-blind clinical trial. Scand J Surg. 2003; 92(2):121-4. PMID: 12841551
33. Walder B, Schafer M, Henzi I, Tramèr MR. Efficacy and safety of patient‐controlled opioid analgesia for acute postoperative pain. Acta Anaesthesiol Scand. 2001; 45(7):795-804. PMID: 11472277 DOI: 10.1034/j.1399-6576.2001.045007795.x
34. Hyllested M, Jones S, Pedersen JL, Kehlet H. Comparative effect of paracetamol, NSAIDs or their combination in postoperative pain management: a qualitative review. Br J Anaesth. 2002; 88(2):199-214. PMID: 11878654 DOI: 10.1093/bja/88.2.199
35. Rّmsing J, Mّiniche S, طstergaard D, Dahl JB. Local infiltration with NSAIDs for postoperative analgesia: evidence for a peripheral analgesic action. Acta Anaesthesiol Scand. 2000; 44(6):672-83. PMID: 10903014 DOI: 10.1034/j.1399-6576.2000.440607.x
36. Rّmsing J, Mّiniche S, Dahl JB. Rectal and parenteral paracetamol, and paracetamol in combination with NSAIDs, for postoperative analgesia. Br J Anaesth. 2002; 88(2):215-26. PMID: 11878655 DOI: 10.1093/bja/88.2.215
37. Soroush A, Khorgami Z, Mobayen M, Mofid R. Evaluation of the effects of perioperative administration of celecoxib on pain management
and the use of narcotic after laparoscopic cholecystectomy. Iran J Surg. 2010; 18(3):27-32.
38. Joshi GP, Viscusi ER, Gan TJ, Minkowitz H, Cippolle M, Schuller R, et al. Effective treatment of laparoscopic cholecystectomy pain with intravenous followed by oral COX-2 specific inhibitor. Anesth Analg. 2004; 98(2):336-42. PMID: 14742366 DOI: 10.1213/01.
ane.0000093390.94921.4a
39. Cheng PG, Lim MJ, Onsiong MK, Chiu KY, Chan MK, Li KW, et al. Celecoxib premedication in post-operative analgesia for laparoscopic cholecystectomy. Acute Pain. 2004; 6(1):23-8. DOI: 10.1016/j.acpain.
2004.01.003
40. Ariana M, Rafiei M. Comparison of intraperitoneal bupivacaine and intravenous petidine on postoperative pain after laparoscopic cholecy-stectomy. Iran J Surg. 2010; 17(4):21.
41. Arya B, Abdollahi AA, Golalipour MJ, Kazemnezhad K, Mohammadi M. Evaluation of post operative analgesic efficacy of intramuscular Meperidine, compared to indometacin and diclofenac Na suppositories in unilateral inguinal hernioplasty patients. J Med Sci. 2007; 7(2):311-4.
42. Alamshahi F, Fateh A, Talebi H, Norouzi A, Fateh S. Effect of preoperative gabapentin in reducing pain after laparoscopic cholecystectomy. Anesthesiol Pain. 2012; 3(3):16.
43. Soroori ZZ, Sharami SH, Heidarzadeh A, Shokri L. The comparison between suppository diclofenac and Meperidine in post-cesarean section pain relief: a randomized controlled clinical trial. JRMS. 2006; 11(5):292-6.
44. Meperidine (meperidine): drug information. Waltham, MA: UpToDate; 2018.
45. Ammori BJ, Davides D, Vezakis A, Martin IG, Larvin M, Smith S, et al. Day-case laparoscopic chole-cystectomy: a prospective evaluation of a 6-year experience. J Hepatobiliary Pancreat Surg. 2003; 10(4):303-8. PMID: 14598151 DOI: 10.1007/
s00534-002-0807-6
46. Novacek G. Gender and gallstone disease. Wien Med Wochenschr. 2006; 156(19-20):527-33. PMID: 17103289 DOI: 10.1007/s10354-006-0346-x
47. Nooromid MJ, Blay E Jr, Holl JL, Bilimoria KY, Johnson JK, Eskandari MK, et al. Discharge prescription patterns of opioid and nonopioid analgesics after common surgical procedures. Pain Rep. 2018; 3(1):e637. PMID: 29430565 DOI: 10.1097/PR9.
0000000000000637
48. Abdulla S, Eckhardt R, Netter U, Abdulla W. Randomized, double-blind, placebo-controlled study to assess the efficacy of nonopioid analgesics on pain following arthroscopic knee surgery. Pain Res
Treat. 2012; 2012:305821. PMID: 23213511 DOI: 10.1155/2012/305821
49. Abdulla S, Eckhardt R, Netter U, Abdulla W. A randomized, double-blind, controlled trial on non-opioid analgesics and opioid consumption for postoperative pain relief after laparoscopic cholecystectomy. Acta Anaesthesiol Belg. 2012; 63(1):43-50. PMID: 22783709
50. Taghizadeh H, Sohrabi Z, Mahaki B. A study on efficacy of meperidine hydrochloride and diclofenac sodium (diclen) on pain severity after cesarean section. J Ilam Univ Med Sci. 2007; 14(4):7-12.
51. Abdollahi A, Arya B, Vakili M. Evaluation of postoperative analgesic effect of intramuscular Pethedine, compared to Indomethacin and Diclofenac Sodium suppositories in pain relief after inguinal hernioplasty patients. Arak Med Univ J. 2003; 6(3):40-4.
52. Abdolrazaghnejad A, Banaie M, Tavakoli N, Safdari M, Rajabpour-Sanati A. Pain Management in the emergency department: a review article on options and methods. Adv J Emerg Med. 2018; 2(4):e45. PMID: 31172108 DOI: 10.22114/AJEM.v0i0.93
Received: 2018/06/6 | Accepted: 2019/09/17 | Published: 2019/11/2
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |






