BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
URL: http://jsurgery.bums.ac.ir/article-1-168-en.html
A massive squamous cell carcinoma on the tip of the nose
1Assistant Professor, Department of Anesthesiology, Faculty of Medicine, Birjand University of Medical Sciences, Birjand, Iran
Received: October 19, 2018 Revised: November 27, 2018 Accepted: May 21, 2019
|
Abstract Squamous Cell Carcinoma (SCC) is the second most common skin cancer after basal cell carcinoma. It is aggressive and has metastasis capability; therefore, timely diagnosis can prevent the occurrence of metastasis. There are some treatments available for SCC, such as radiotherapy, topical chemotherapy, systemic chemotherapy, and surgery. In our case, the surgical treatment and radiotherapy were performed due to the results of the examination reports and large dimensions of the lesion. Key words: Carcinoma, Nose, Squamous Cell |
Introduction
Squamous Cell Carcinoma (SCC) is the second most common skin cancer after Basal Cell Carcinoma (BCC) (1). The SCC accounts for 20% of skin cancers (2). Moreover, more than 700.000 new cases are detected annually in the United States (3). The risk factors contributing to this disease include sun exposure, age (in the mid-60's), and gender (i.e., it is 3 times more common in male than female) (4). Another risk factor is contact with carcinogenic chemicals (2). Although most SCCs can be treated, it has already been stated that 14% of them develop metastases, out of which 40% of the cases will finally turn to be fatal (2). Accordingly, timely diagnosis is crucial to the survival of the patients. In this report, we presented a case with a massive SCC on the tip of his nose.
Cases
The patient was a 48-year-old male referring to the hospital with a medical history of smoking and exposure to sunlight. On physical examination, it was found that the lesion had begun to grow gradually over the last six months and it turned into a volcano-shaped lesion without pain. In addition, no similar symptoms were observed in his family history and there were no abnormalities after pharynx and larynx examination. After conducting the necessary examinations, the patient underwent two surgeries. The first surgery was excision biopsy, the result of which was SCC. Afterward, during the second operation, the lesion was completely removed under general anesthesia (Figure 1). Figure 1 presents a huge lesion with dimensions of 5×4 cm. Due to the large dimensions of the lesion, the transitional flap was performed (Figure 2). Eventually, in order to continue the treatment, the patient was referred to undergo radiotherapy. In the past four months, the skin examinations were performed, and no problems were noticed in this case report.
Discussion
The SCC is the second most common skin cancer and it appears frequently on parts of the body exposed to sunlight, such as head, face, and neck. In our case, the skin lesion was on the tip of the nose. There are some risk factors contributing to this disease, such as carcinogen substances, chronic skin wounds, ultraviolet radiation, age,


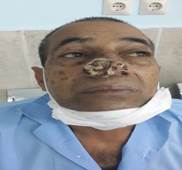
Figure 1: A large Squamous Cell Carcinoma on the nose (preoperative)



Figure 2: Removed lesion (postoperative)
and gender (3, 5). Except for age, all factors were present in our case. Although SCC is the second most common skin cancer after BCC, it is aggressive and has metastasis capability. Due to this feature, timely diagnosis can prevent the occurrence of metastasis (6). In the case presented, cancer was diagnosed early and had no metastasis. Moreover, in our case, no metastasis was found according to the results obtained from the examination of neck lymph nodes and computed tomography scan (7). There are some treatments for SCC, including radiotherapy, topical chemotherapy, systemic chemotherapy, and surgery (8). In our case, the surgical treatment and radiotherapy were performed due to the results of examination and dimensions of the lesion.
Conclusions
In SCC skin cancer, timely diagnosis is crucial in order to prevent the metastasis. In addition, regular skin examination is necessary. It is clear that the utilization of sun protection strategies is essential for those who are exposed to the sun.
Conflict of Interest
There are no conflicts of interest regarding the publication of the study.
References
1. Dye K, Saucedo M, Raju D, Aydin N. A common cancer in an uncommon location: a case report of squamous cell carcinoma of the nipple. Int J Surg Case Rep. 2017; 36:94-7. PMID: 28551484 DOI: 10.1016/j.ijscr.2017.05.020
2. Voiculescu V, Calenic B, Ghita M, Lupu M, Caruntu A, Moraru L, et al. From normal skin to squamous cell carcinoma: a quest for novel biomarkers. Dis Markers. 2016; 2016:4517492. PMID: 27642215 DOI: 10.1155/2016/4517492
3. Davis J, Bordeaux J. Squamous cell carcinoma. JAMA Dermatol. 2013; 149(12):1448. PMID: 24352728 DOI: 10.1001/jamadermatol.2013.6947
4. Que SKT, Zwald FO, Schmults CD. Cutaneous squamous cell carcinoma Incidence, risk factors, diagnosis, and staging. J Am Acad Dermatol. 2018; 78(2):237-247. PMID: 29332704 DOI: 10.1016/j.
jaad.2017.08.059
5. Yan W, Wistuba II, Emmert-Buck MR, Erickson HS. Squamous cell carcinoma-similarities and differences among anatomical sites. Am J Cancer Res. 2011; 1(3):275-300. PMID: 21938273
6. Renzi C, Mastroeni S, Mannooranparampil TJ, Passarelli F, Caggiati A, Potenza C, et al. Delay in diagnosis and treatment of squamous cell carcinoma of the skin. Acta Derm Venereol. 2010; 90(6):595-601. PMID: 21057742 DOI: 10.2340/00015555-0966
7. Becker M, Zaidi H. Imaging in head and neck squamous cell carcinoma: the potential role of PET/MRI. Br J Radiol. 2014; 87(1036):20130677. PMID: 24649835 DOI: 10.1259/bjr.20130677
8. Potenza C, Bernardini N, Balduzzi V, Losco L, Mambrin A, Marchesiello A, et al. A review of the literature of surgical and nonsurgical treatments of invasive squamous cells carcinoma. Biomed Res
Int. 2018; 2018:9489163. PMID: 29808169 DOI: 10.1155/2018/9489163
Received: 2018/10/19 | Accepted: 2019/05/21 | Published: 2019/09/22
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |









