BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
URL: http://jsurgery.bums.ac.ir/article-1-171-en.html
Impact of practice on goat’s eye on surgical skill development in sophomore ophthalmology residents
Mohammad Reza Akhlaghi1![]() , Ali Salehi1
, Ali Salehi1![]() , Ali Akbar Mortazavi1
, Ali Akbar Mortazavi1![]() , Mohammad Shafieion2
, Mohammad Shafieion2![]() , Rezvan Ansari3*
, Rezvan Ansari3*![]()
1Associate Professor, Department of Ophthalmology, Faculty of Medicine, Feiz Teaching Hospital, Isfahan, Iran
2General Physician, Managing Director of Feiz Teaching Hospital, Isfahan University of Medical Sciences, Isfahan, Iran
3MSc in Medical Education, Official in Charge of Educational Accreditation and Education Development Office, Feiz Teaching Hospital, Isfahan University of Medical Sciences, Isfahan, Iran
Received: November 12, 2018 Revised: May 25, 2019 Accepted: May 25, 2019
|
Abstract Introduction: Acquisition of clinical and practical skills is one of the highly critical and sensitive aspects of medical education, particularly in the areas related to surgical specialties. Moreover, one of the most important procedural strategies regarding educational medicine is the acquisition of practical skills in various psychological domains. Regarding this, the present study aimed to delineate the effects of practicing on goat’s eye for the residents expected to perform their first surgery on human eyes. Methods: This applied study was conducted on all the sophomore residents (n=8) of the Ophthalmology Department of Isfahan University of Medical Sciences, Isfahan, Iran, using a pre-experimental design. The procedures were instructed to the residents through three stages in the wet lab according to a protocol. After the completion of the second stage, the residents gained their first experience of performing surgery on human eyes in the operating room under the supervision of junior and senior residents and the attending specialist. At this stage, in case further experience was required, the resident could start practicing on goat’s eyes in the wet lab upon prior coordination. At the third stage, the residents received instructions and practiced more advanced techniques. After this stage and upon the entrance of the residents to the operating room, the 3rd and 4th year residents and the attending specialists were surveyed regarding the performance of the 2nd year residents in nine fields in accordance with the aims of the study. In addition, the 2nd year residents completed a self-evaluation checklist. The data were analyzed in SPSS software, version 16. Results: The results revealed that practicing before surgery on the human eye resulted in the reduction of surgical errors (45%), surgical speed and proficiency (20%), and stress and hand tremors (35%) during the first surgical experiences. According to the 3rd and 4th year residents, the practices and instructions provided before the wet lab had a positive effect on decreasing the levels of stress and surgical error during the first surgical experiences of the 2nd year residents. The attending specialists believed that the wet lab experience could have a positive effect on all aspects of surgery, including mental, emotional, and practical factors. Nonetheless, some 3rd and 4th year residents believed that the wet lab could not provide circumstances identical to the conditions experienced in the operating room. Therefore, the effects of practicing in the wet lab on surgical speed, proficiency, stress, and surgical error were believed to be less significant. Conclusions: Overall, the study showed that repeated practice sessions on goat’s eye in the wet lab under the supervision of 3rd and 4th year residents and attending specialists could not only have positive effects on some practical, mental, and attitudinal indices but also improve the knowledge of the residents. Key words: Education, Goat’s Eye, Resident, Surgery, Wet Lab |
Introduction
Skill training has an essential share in medical education. The acquisition of clinical and practical skills is one of the highly critical and sensitive aspects of medical education, particularly in surgical specialties. Moreover, one of the most significant procedural strategies regarding educational medicine is the acquisition of practical skills in various psychological domains (1). The skills that a specialist possesses are strongly related to the methods and amount of education she/he has received and practiced during the educational period of medical practice (2).
The acquisition of skills and experimental aspects is a dynamic process in which the learner gradually learns through applying logical reasoning to the accumulated experiences on a day to day basis. However, the first experiences can occasionally lead to irreversible consequences for patients (3). Based on the evidence, in 85% of cases, residents gaining advanced experience through educational surgical procedures make errors that have, in some cases, caused irrecoverable damages to the patients.
Regarding this, the attending specialists always seek for ways to simulate the operating room (OR) experience in order to prevent such errors. However, given the costliness of these simulations, universities have to discontinue these projects (4). Moreover, simulation-based learning has been so costly that the majority of universities have been oriented toward adopting animal eyes in the wet labs for students’ primary surgical experiences (5). According to the literature, the use of wet labs is an appropriate educative surgical method to practice and learn before the OR experience that can help develop surgical proficiency, especially in the residents of surgery (6-7).
Wet labs provide a safe and stress-free environment in which the residents of surgery can familiarize themselves with surgical techniques and gain the needed confidence to perform surgery on humans. Special instructions are provided for the residents in the wet labs; moreover, they can learn about the multitudes of surgical tools available in this setting (8).
The delicate structure of the eye tissues and the small size of the anatomical parts of the eye all underscore the necessity of acquiring surgical proficiency in the residents of surgery before performing surgery on actual human eyes. In
other words, to perform a multi-stage cataract procedure, residents should gain the needed skills in the wet labs by performing the procedure on simulated eyes or animal eyes that have an anatomical resemblance to the human eye. Studies have shown that practice sessions and skills acquired in the wet labs by residents have decreased the number of errors occurring during human surgeries by 10% (9-16).
On the other hand, the residents of surgical fields, in which the acquisition of the required skills for performing surgical procedures is of utmost importance, are faced with much stress and anxiety that can increase the risk of irrecoverable errors (17). Given the ultimate goals of education and learning, the empowerment of medical students and residents has a positive effect on maintaining and enhancing public health (17).
The implementation of a safe procedure on patients by the attendance of a specialist is a major educational goal. Alongside this, teachers have frequently attempted to provide appropriate conditions for eye simulation, such as the use of animals eyes (e.g., cows, pigs, sheep, and goats). In the universities across the world, pigs’ eyes are widely available as they have a similar anatomical structure to the human eye (18-19).
The acquisition of the first experiences of surgical procedures using similar models (i.e., animal models) is a method that has been able to decrease surgical risks and errors in human patients. Moreover, the use of these animal models facilitates the reduction of the stress level of residents in their first experiences of performing surgery on human eyes and the improvement of their sense of confidence and motivation.
Consequently, the establishment of a specific program with clear objectives will elevate the educational system and methods. With this background in mind, the present study was conducted to investigate the effects of an appropriate method in the clinical training of the residents of ophthalmology surgery and fix the observed inadequacies during the process.
Methods
This applied study was conducted on sophomore residents (n=8) of the Ophthalmology Department of Isfahan University of Medical Sciences, Isfahan, Iran, using a pre-experimental design. The interventions have been implemented since February 2017 and continue to the present time. During this period, the researchers have enquired about the efficacy of the wet lab in line with the current research objectives.
The study population consisted of all 2nd year residents (n=8) participating in the educational intervention. After the completion of the third stage of the intervention, the participants filled out a self-evaluation questionnaire upon performing at least three surgical procedures on human eyes in the OR. Furthermore, 3rd year (n=8) and 4th year (n=8) residents of the ophthalmology department and the corresponding attending specialists of the OR completed a surveying checklist (similar to the self-evaluation form of the 2nd year residents).
The latter survey was performed to assess the performance of the 2nd year residents in their first experiences of surgery on human eyes. A total of 70 forms were completed by junior and senior residents given that each 2nd year resident was evaluated by three higher-level residents, as well as the attending specialist.
The data collection tools comprised of three survey forms each of which included nine items. The participants were asked individually to score each of the items on a 5- point Likert scale (completely disagree=1 to completely agree=5). This form was confirmed to be valid by three faculty members and two residents of the ophthalmology department. The reliability of the checklist was also tested through administering it to five residents, rendering a Cronbach’s alpha coefficient of 0.75. The forms had similar contents and were designed with two contexts in mind to be completed by an observer and a supervisor of the performance.
The study was conducted in the wet lab and the OR of Feiz medical and educational center specializing in eye diseases affiliated to the Isfahan University of Medical Sciences. The residents were evaluated for 3 months at specified intervals. According to the literature, six stages are required to establish a wet lab. These stages include the establishment of appropriate physical conditions, presence and support of
the faculty members of the ophthalmology department and an office worker who is persistent and informed, provision of appropriate eye models or simulated eyes, adoption of an appropriate method for fixing the eye while practicing surgery, preparation of the eye in the sense of inducing cataract in the eye under study, and financial support for the preliminary costs of running the wet laboratory and its machines, as well as usable materials including the simulated eyes or eyes of animals.
At first, the researcher coordinated with the hospital officials and the ophthalmology department in February 2018 for a room in the Feiz Medical and Educational Ophthalmology Center in which the wet lab instruments could be designed and set. The required facilities were transferred after setting up the cabinets, electricity and telephone systems, and plumbing, cooling, and heating equipment in the room (Table 1).
The researchers used the goat’s eye because of its similarity with the human eye. Investigations of different databases, including the PubMed, and search engines regarding wet labs revealed that researchers had reached different conclusions about the type of simulated eye for practicing in the wet lab. This was the beginning phase of deciding on the type of eye most similar to the human eye, which can be available in Islamic countries.
As the evidence indicates, the pig’s eye is used as the most similar eye to the human eye and is regarded as an appropriate reference in wet labs (20-21). Nevertheless, in a study carried out in India, it was shown that the goat’s eye was an appropriate option for practicing purposes in the wet labs (22). In another study performed by Mohammadi in the Eye Research Center in Iran, sheep’s eye was suggested as an appropriately similar model to the human eye (23). In the current study, goat’s eyes were adopted given their simple accessibility and cost-effectiveness, as well as more similarity with human eyes.
To provide the eyes, the slaughterhouse (in Khomeini Shahr, 80 km to Isfahan) was asked to totally extract the eyes from the animal's eye orbit, along with the surrounding fat, without the eye
Table 1: Facilities and equipment required for a wet laboratory
|
Row |
Item |
|
1 |
Surgical microscope with a teaching tube (Topcon trademark) |
|
2 |
Fico ARC machine |
|
3 |
Microwave |
|
4 |
Trypan Blue |
|
5 |
An extra set, including blepharostat, tying, Westcott scissors, corneal scissors, forceps, and … |
|
6 |
Phacoemulsification sets, including blepharostat, chopper, irrigation and aspiration system, phaco tip, Sinskey hook, tooth forceps, and pencil capsule |
|
7 |
Surgical instruments, including knife 2/3 and 15 degrees, suture (0.6, 0.7, and 10.0), sterile insulin syringe, and gel |
|
8 |
Bed and suitable sandals |
|
9 |
Small fridge |
|
10 |
Safety box |
|
11 |
Yellow bucket (for infectious waste) |
Table 2: Practicable procedures in the wet lab
|
Row |
Procedure |
|
1 |
Correct scrubbing and handwashing |
|
2 |
Familiarity with the eye surgery |
|
3 |
Learning how to adjust the microscope |
|
4 |
Learning how to insert stab |
|
5 |
Learning how to wash the anterior chamber |
|
6 |
Gel injection and dyeing of the anterior capsule |
|
7 |
Performing a rhexis (capsulorhexis) |
|
8 |
Performing phacoemulsification |
|
9 |
Irrigation and aspiration |
|
10 |
Intra-ocular lens |
|
11 |
Stromal hydration |
|
12 |
Eye stitching |
surface being touched. The eyes were transferred to the wet lab in a cold container at -2°C. Notably, the slaughterhouse was visited every day by the researcher to supervise the process of eye preparation and ensure that they are completely intact and immediately placed in appropriate conditions in 1/3 and 2/3 sera at -2°C.
The eyes were used in the wet lab on the same day. The maximum time interval from the moment the eye was extracted from the socket of the animal skull until it was used in the wet lab was 10 h. The eyes were transferred in such conditions in order to prevent the cornea from getting opaque or dry and preserve maximum similarity to the human eye needed in the wet lab.
It is worthy of note that all these procedures (Table 2) were taught to the residents in three separate stages. In this regard, items 1-3 were taught to the residents by a 3rd year resident in the first 2 weeks of the educational program. In addition, items 4-6 were instructed by 3rd and 4th year residents in two sessions with a one-week interval.
In the first session of the educational program, the higher grade residents performed the procedure on the eye model as an example for the 2nd year residents to follow. By observing the procedure, they attempted the procedure under the supervision of the higher grade resident. There was a one-week interval before the second session during which the 2nd year residents had the opportunity to study the topic and review it in their minds.
The 2nd year residents performed the 4th-6th procedures under the supervision of higher grade residents in the second session. After this stage, the newly trained residents practiced the procedures on their own or with their colleagues in the wet lab. After acquiring the required skills, they were permitted into the OR to hold the scalpel and perform the surgery on the human eye under the supervision of attending specialists, as well as 3rd and 4th year residents according to the rotation schedule of the OR.
During this period, if it was sensed or observed (whether by the 2nd year residents themselves
or by the attending specialist or higher grade residents) that there is a need for more practice in the wet lab, coordination was immediately made for the 2nd year residents to have more practice sessions on goat’s eyes.
Regarding the third stage of the educational program, after the target residents had practiced in the OR for 2-3 sessions and performed the practices specified in the first stage, they were again met at the wet lab (according to a written schedule). This meeting was aimed at both solving the problematic issues and getting trained on procedures 7-11 (based on Table 2).
Subsequently, they started practicing on goat’s eye and reiterated the previous procedures on humans under the supervision of higher-grade residents and the attending specialist. The survey forms were completed by the study group after the end of stage 3. The collected data were analyzed
in SPSS software, version 16. Notably, the intervention used in this study was the routine education delivered to all residents of surgery in the hospitals affiliated to the Isfahan University of Medical Sciences.
Results
As seen in Figure 1, the 2nd year residents believed that the exercises performed on animal eyes in the wet lab could have a positive effect
on the residents’ confidence (65%), surgical proficiency (70%), motivation while operating on the human eye (80%), satisfaction with operation (70%), self-esteem (55%), and mentality towards surgical operation and mental ability in performing surgical operation (80%). In their opinion, however, these exercises were of a lower effect on surgical error (45%), agility (20%), and stress and hand tremors while operating for the first time (35%; Figure 1).
In the same vein, the supervising residents maintained that the exercises performed on animal eyes in the wet lab had a positive effect on confidence (85%), surgical proficiency (95%), reduction of surgical errors (85%), motivation while operating on the human eye (80%), satisfaction while operation (70%), self-esteem (85%), and positive mentality and ability in performing the surgical operation (100%) in the 2nd year residents. Nevertheless, these pre-operative exercises had a weaker effect on agility (40%) and stress and hand tremor while operating on the
human eye for the first time (40%; Figure 2).
As depicted in Figure 3, in some cases, the attending specialists had different opinions from those of junior and senior residents regarding the wet lab. In this regard, the attending specialists believed that practicing on animal eyes had a positive effect on confidence (80%), surgical proficiency (85%), surgical error (50%), motivation while operating on the human eye (85%), satisfaction with operation (70%), self-esteem (95%), and positive mentality and ability in surgical operation (100%) in the 2nd year residents.

Figure 1: Self-assessment of sophomore residents about the efficacy of first experience with surgery on goat’s eye
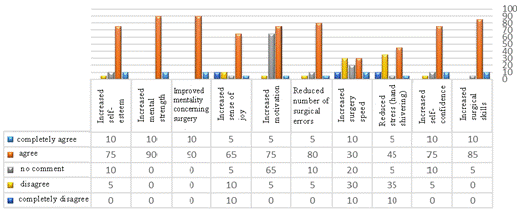
Figure 2: Assessment of junior and senior residents’ viewpoints about the efficacy of the first surgical experience of sophomore residents on goat’s eye
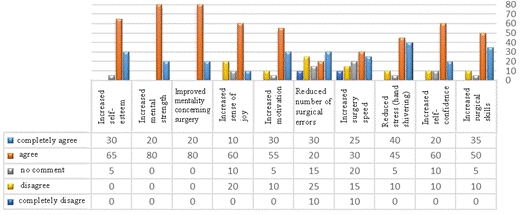
Figure 3: Assessment of attending specialists’ viewpoints about the efficacy of the first surgical experience of sophomore residents on goat’s eye
Moreover, the specialists assumed that the pre-operative exercises had a significant impact on agility (55%) and stress and hand tremors (85%) during the first operation on human eyes.
Discussion
Many studies have been published regarding the importance of surgical simulation exercises. The results of all of these investigations are indicative of an improvement in the learners’ surgical proficiency in real-life situations and on humans (10-12). Based on the residents’ self-evaluation, the implementation of these exercises prior to OR experience on humans had weaker effects on surgical error (45%), agility (20%), and stress and hand tremors (35%) during the first surgical experience.
Similar studies on practicing with the pig’s eye have shown that such practices before surgical operation on the human eye reduced the residents’ surgical errors by ten times and increased the required confidence for operation on human eyes (14, 16).
In similar studies (8, 22-25), 80% of the ophthalmology residents stated that the practice and acquisition of the skills required for operation on animal eyes in the wet lab positively contributed to all dimensions of operation on human eyes. When questioned about whether the instruments available at the wet lab were sufficient and appropriate, 60% of the residents stated that goat’s eye had many similarities to human’s eye. They also affirmed that the instruments in the wet lab were appropriate for surgery.
Overall, studies have shown that wet labs have positive effects by facilitating the implementation of simple, safe, and cost-effective education through which the residents can acquire the skills needed for eye surgery.
Although most of the 3rd and 4th year residents in the present study did not have the wet lab experience, they stated that the exercises and instructions provided before the wet lab could positively affect their performance, stress, and error. The attending specialists believed that the wet lab could have positive effects on mental, emotional, and professional aspects. Nonetheless, some higher-level residents maintained that the wet lab cannot render a completely similar condition to that of the OR and that practically, it has a lower effect on agility, error, and stress.
The results of a quasi-experiential study conducted in 2018 on interns showed that the students trained in skills laboratory had a higher scientific ability and confidence than those going through traditional methods when present at the patient’s bed in real-life clinical settings (18). In
a study addressing the medical students’ evaluation of the quality of education provided at the clinical skills laboratory in Gilan, Iran, the results showed that most of the students were not satisfied with the quality of the education provided. However, they rated such centers as highly effective in preparing the students
for subsequent presence in real-life clinical circumstances (17).
While wet labs play an important role in educating eye surgery residents, there are limitations in collecting the eye samples, which are completely identical to the human eye in anatomical structure. Differences in the frontal chamber, corneal structure, thick and elastic capsule, and big soft lenses are some of the variations present in the eyes similar to the human’s eye. Despite such limitations, the wet labs are regarded as the most essential and practical alternatives for surgical exercises before operating the human eye.
Conclusions
As the findings indicated, repeated practice in the wet lab under the supervision of higher-level residents and attending specialists can have very positive effects on some professional, mental, attitudinal, and even knowledge-based indices. Consequently, it is recommended to increase the efficiency of these laboratories by extending practice sessions and opportunities.
Acknowledgments
This study was a team effort, and it is essential to give our sincerest appreciations to the manager of the hospital, namely Dr. Shafi’iun. Another thanks go to Mr. Khalili Moghaddam, and the person responsible for procuring goat’s eyes, Mr. Mehrshad.
Funding
The financial sources involved the instruments and facilities available at Feiz Medical Educational Eye Center. In addition, the materials and goat’s eyes were prepared using the fund from the hospital.
Conflict of Interest
This study does not have any conflicts of interest with any organization or institution.
References
1. Razavy SM, Salamati P, Shahgholi E, Honarmand M, Rahbarimanesh AA, Alehossein M, et al. The effects of clinical skills learning centers on learning promotion among pediatrics interns. Iran J Med Educ. 2011; 10(4):430-8. [Persian]
2. Ramezani M, Kermanshahi S. A survey of the quality of clinical education in nursing. J Jahrom Univ Med Sci. 2011; 9(1):14-21. [Persian]
3. Ahmadinezhad Z, Ziyaee V, Morvejee A. Tehran University of Medical Interns' satisfaction from the quality of clinical education by job satisfaction standard forms. J Med Educ. 2002; 7:8-9. [Persian]
4. Sanatkhani M, Molla M, Akbari M. Evaluation of the students’ perception about clinical education and examination in Mashhad school of dentistry (Iran) in 2009. J Mashhad Dent Sch. 2012; 36(3):211-22. [Persian]
5. Sharifi B, Ghafarian Shirazi HR, Momeninejad M, Saniee F, Hashemi N, Jabarnejad A, et al. A survey of the quality and quantity of clinical education from the viewpoint of medical students. J Jahrom Univ Med Sci. 2012; 10(2):57-63. [Persian]
6. Qayumi AK, Cheifetz RE, Forward AD, Baird RM, Litherland HK, Koetting SE. Teaching and evaluation of basic surgical techniques: the University of British Columbia experience. J Invest Surg. 1999; 12(6):341-50. PMID: 10630398
7. Velmahos GC, Toutouzas KG, Sillin LF, Chan L, Clark RE, Theodorou D, et al. Cognitive task analysis for teaching technical skills in an inanimate surgical skills laboratory. Am J Surg. 2004; 187(1):114-9. PMID: 14706600
8. Lee AG, Greenlee E, Oetting TA, Beaver HA, Johnson AT, Boldt HC, et al. The Iowa ophthalmology wet laboratory curriculum for teaching and assessing cataract surgical competency. Ophthalmology. 2007; 114(7):e21-6. PMID: 17475332 DOI: 10.1016/j.
ophtha.2006.07.051
9. Oetting TA, Lee AG, Beaver HA, Johnson AT, Boldt HC, Olson R, et al. Teaching and assessing surgical competency in ophthalmology training programs. Ophthalmic Surg Lasers Imaging. 2006; 37(5):384-93. PMID: 17017198
10. Albanis CV, Dwyer MA, Ernest JT. Outcomes of extracapsular cataract extraction and phacoemul-sification performed in a university training program. Ophthalmic Surg Lasers. 1998; 29(8):643-8. PMID: 9715489
11. Badoza DA, Jure T, Zunino LA, Argento CJ. State-of-the-art phacoemulsification performed by residents in Buenos Aires, Argentina. J Cataract Refract Surg. 1999; 25(12):1651-5. PMID: 10609212
12. Hennig A, Schroeder B, Kumar J. Learning phacoemulsification. Results of different teaching methods. Indian J Ophthalmol. 2004; 52(3):233-4. PMID: 15510464
13. Misra A, Burton RL. Incidence of intraoperative complications during phacoemulsification in vitrectomized and nonvitrectomized eyes: prospective study. J Cataract Refract Surg. 2005; 31(5):1011-4. PMID: 15975471 DOI: 10.1016/j.jcrs.2004.10.052
14. Prasad S. Phacoemulsification learning curve: experience of two junior trainee ophthalmologists. J Cataract Refract Surg. 1998; 24(1):73-7. PMID: 9494902
15. Robin AL, Smith SD, Natchiar G, Ramakrishnan R, Srinivasan M, Raheem R, et al. The initial complication rate of phacoemulsification in India. Invest Ophthalmol Vis Sci. 1997; 38(11):2331-7. PMID: 9344356
16. Thomas R, Naveen S, Jacob A, Braganza A. Visual outcome and complications of residents learning phacoemulsification. Indian J Opthalmol. 1997; 45(4):215-9. PMID: 9567016
17. Mardani M, Shams M, Mosadegh AA, Rezapoor S. Effectiveness of training programs' clinical skills of emergency "on learning of medical students. J Lorestan Univ Med Sci. 2010; 12(3):45-50. [Persian]
18. Razavy SM, Salamati P, Shahgholi E, Honarmand M, Rahbarimanesh AA, Alehossein M, et al. The effects of clinical skills learning centers on learning promotion among pediatrics interns. Iran J Med Educ. 2011; 10(4):430-8. [Persian]
19. Khoshrang H, Salari A, Dadgaran I, Moaddab F, Rouhi Balasi L, Pourkazemi I. Quality of education provided at the clinical skills laboratoryfrom medical students’ viewpoints in Guilan University of medical sciences. Res Med Educ. 2016; 8(2):72-83. DOI: 10.18869/
acadpub.rme.8.2.77
20. Henderson BA, Grimes KJ, Fintelmann RE, Oetting TA. Stepwise approach to establishing an ophthalmology wet laboratory. J Cataract Refract Surg. 2009; 35(6):1121-8. PMID: 19465299 DOI: 10.1016/j.
jcrs.2009.01.027
21. William RW, Arora S, Kutzner M, Damji KF. Porcine cataract creation using formalin or microwave treatment for an ophthalmology wet lab. Can J Ophthalmol. 2016; 51(4):244-8. PMID: 27521661 DOI: 10.1016/j.jcjo.2016.01.012
22. Ramani S, Pradeep TG, Sundaresh DD. Effect of wet-laboratory training on resident performed manual small-incision cataract surgery. Indian J Ophthalmol. 2018; 66(6):793-7. PMID: 29785985 PMCID: PMC5989499 DOI: 10.4103/ijo.IJO_1041_17
23. Mohammadi SF, Mazouri A, Jabbarvand M, Rahman-A N, Mohammadi A. Sheep practice eye for ophthalmic surgery training in skills laboratory. J Cataract Refract Surg. 2011; 37(6):987-91. PMID: 21596242 DOI: 10.1016/j.jcrs.2011.03.030
24. Pilling RF, Bradbury JA, Reddy AR. Strabismus surgical skills assessment tool: Development of a surgical assessment tool for strabismus surgery training. Am J Ophthalmol. 2010; 150(2):275-8. PMID: 20541739 DOI: 10.1016/j.ajo.2010.03.007
25. McClatchey SK, Lane RG, Kubis KC, Boisvert C. Competency checklists for strabismus surgery
and retinopathy of prematurity examination. J
AAPOS. 2012; 16(1):75-9. PMID: 22370670 DOI: 10.1016/j.jaapos.2011.09.008
Received: 2018/11/12 | Accepted: 2019/05/25 | Published: 2020/03/4
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |









